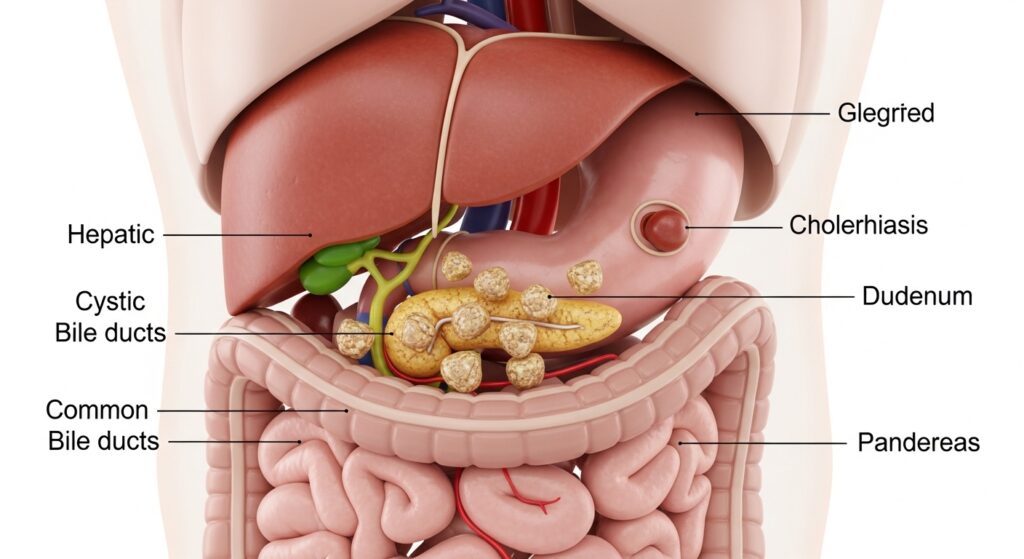
Someone searching for “Cholerhiasis” is most likely trying to understand a medical condition—what it is, why it happens, how serious it is, and what to do about it. In many cases, this term appears to be a misspelling or variation of Cholelithiasis, which refers to the formation of gallstones in the gallbladder.
This article is structured to help you:
- Understand the condition clearly
- Recognize symptoms early
- Learn real-life management strategies
- Make informed decisions about treatment
What Is Cholerhiasis?
Cholerhiasis (likely referring to cholelithiasis) is a condition where solid particles—called gallstones—form in the gallbladder. The gallbladder is a small organ beneath the liver that stores bile, a digestive fluid.
These stones can vary in size—from tiny grains to large stones—and may or may not cause symptoms.
What Causes It?
Gallstones form when bile becomes imbalanced. The most common causes include:
- Excess cholesterol in bile
- Too much bilirubin (a waste product from red blood cells)
- Poor gallbladder emptying
- Genetic predisposition
Risk Factors
- Obesity or rapid weight loss
- High-fat diet
- Diabetes
- Pregnancy
- Age (more common after 40)
Types of Gallstones
- Cholesterol Stones
- Most common
- Yellow-green in color
- Pigment Stones
- Smaller and darker
- Linked to liver disease or blood disorders
Symptoms: When to Worry
Many people with cholerhiasis have no symptoms. But when stones block bile flow, symptoms appear.
Common Signs
- Sudden pain in upper right abdomen
- Pain after fatty meals
- Nausea and vomiting
- Back or shoulder pain
Serious Complications
If untreated, it can lead to:
- Cholecystitis (inflamed gallbladder)
- Pancreatitis
- Bile duct blockage
Real-World Example
A 42-year-old office worker begins experiencing sharp abdominal pain after eating fried food. Initially ignored, the pain worsens and leads to an emergency visit. Ultrasound reveals multiple gallstones. After recurring attacks, doctors recommend surgery.
This is a typical progression when early symptoms are overlooked.
Diagnosis
Doctors usually confirm the condition through:
- Ultrasound (most common)
- CT scan (for complications)
- Blood tests (to detect infection or blockage)
Treatment Options
1. Watchful Waiting
If there are no symptoms:
- No immediate treatment needed
- Regular monitoring
2. Medications
Some cases use bile acid pills like Ursodeoxycholic acid
- Works slowly
- Not effective for all types
3. Surgery (Most Common)
Procedure: Cholecystectomy
- Removes the gallbladder entirely
- Minimally invasive (laparoscopic)
- Quick recovery
Practical Use Cases: Managing Daily Life
Diet Adjustments
- Reduce fried and fatty foods
- Increase fiber (vegetables, oats)
- Stay hydrated
Lifestyle Changes
- Maintain a healthy weight
- Avoid crash dieting
- Exercise regularly
After Surgery
- Most people live normally without a gallbladder
- Some may need to adjust diet temporarily
Comparison: Treatment Options
| Option | Best For | Pros | Cons |
|---|---|---|---|
| Watchful Waiting | No symptoms | No intervention needed | Risk of sudden attack |
| Medication | Small cholesterol stones | Non-surgical | Slow, limited effectiveness |
| Surgery | Frequent symptoms | Permanent solution | Requires procedure |
Pros and Cons of Treating Cholerhiasis
Pros
- Relief from pain and discomfort
- Prevents complications
- Improves quality of life
Cons
- Surgery risks (though minimal)
- Possible digestive adjustments post-surgery
- Medication may not always work
Frequently Asked Questions (FAQ)
1. Is cholerhiasis dangerous?
It can be if complications develop. Many cases remain harmless unless symptoms appear.
2. Can gallstones go away on their own?
Rarely. Most persist unless treated.
3. What foods trigger symptoms?
Fatty, fried, and greasy foods are the most common triggers.
4. Is surgery always required?
No. Only symptomatic or complicated cases need surgery.
5. Can I live normally without a gallbladder?
Yes. The body adapts, and digestion continues normally for most people.
Final Thoughts
Cholerhiasis (cholelithiasis) is common but manageable. The key is early awareness and informed decision-making. If you experience recurring abdominal pain—especially after meals—it’s worth getting checked.
With proper care, lifestyle adjustments, and medical guidance, most people handle this condition without major disruption to their lives.